Understanding Periodontal Abscess: Symptoms, Causes, and Treatments
Periodontal Abscess is a pus-filled area that develops when an infection affects a particular area of the mouth. A periodontal abscess in this situation, also known as a lateral abscess, is one that affects the teeth and other oral bony structures. You can get knowledge about symptoms, causes, treatments as well as how to prevent them below this article.
Keeping this guide to get information about Periodontal Abscess!
Overview of Periodontal Abscess
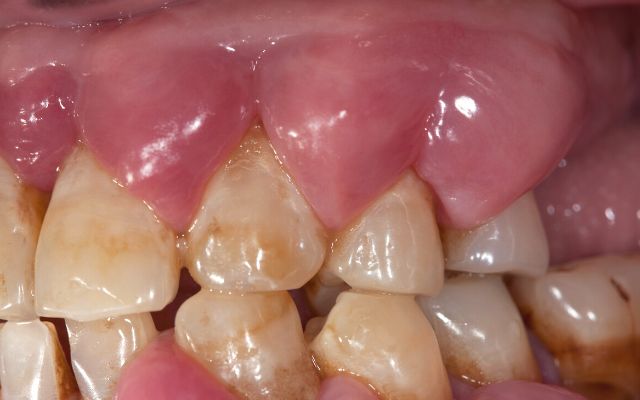

A periodontal abscess is a critical condition that demands attention within the realm of dentistry. It manifests as a localized infection, characterized by the formation of a pus-filled pocket in the connective tissues surrounding the affected tooth. This condition poses significant challenges and requires comprehensive understanding for effective management.
Periodontal abscesses typically arise from the progression of periodontal disease, wherein the infection spreads to the deeper structures supporting the teeth. The underlying cause often involves the buildup of plaque and calculus, leading to bacterial invasion and subsequent inflammation. Factors such as poor oral hygiene, compromised immune response, and anatomical factors may contribute to the development of periodontal abscesses.
Types of Gum Abscess
In addition to periodontal abscess, the following two types of dental abscess exist:
- Gingival abscess: This type of abscess affects only the gingival (gum) tissue. It may be located very close to the tooth, but it is not caused by a tooth infection.
- Abscess periapical: A periapical abscess begins with an infection of the dentin in the tooth’s soft pulp, oral cavity, periapical abscesses
The symptoms of both of these abscesses resemble those of periodontal abscess and skin abscesses, systemic antibiotics.
The Symptoms Of A Periodontal Abscess
Periodontal abscess patients may suffer mild to severe pain. When touching the abscess, the patient will experience pain; sensitive teeth, teeth that move or protrude; a bad taste in the mouth, local lymph node enlargement, fever, and malaise.
As the patient is in an acute inflammatory condition, these symptoms are more prevalent, but when drainage occurs, the abscess becomes chronic, and the symptoms diminish: periodontics, periodontal diseases, periodontal ligament (pdl),
Pain is the primary symptom of a periodontal abscess, but there are additional warning signs.
- Increased pressure and pain when lying down.
- Heightened sensitivity to the temperature of food and drink
- A rush of foul-tasting liquid upon biting, accompanied by a temporary reduction in pain.
- Poor breath
- Trouble swallowing
- General malaise or a feeling of being “off” or ill.
- Fever
- Pain that radiates to the ear, jaw, and neck.
Additionally, in extreme cases, periodontal abscesses can cause breathing difficulties. At this point, it is crucial to seek medical attention immediately. If you are unable to schedule an appointment with your dentist or primary care physician, a weekend dentist can assist you.
If none of these alternatives are available, you should visit an emergency dentist or the emergency room.
Initially, a dental abscess may not cause any pain, and pain may be episodic as the abscess swells and bursts repeatedly. Patients may experience a period without pain, followed by a gradual increase in pressure and discomfort in the affected tooth.
How Threatening Is A Tooth Abscess?


Irrespective of whether you have a periodontal abscess, a gingival abscess, or a parietal abscess, it is crucial that you receive prompt treatment.
If left untreated, an abscessed tooth can result in more serious health complications, such as:
- Sinusitis infection
- A fistula is the bony and skin formation of a hollow tunnel.
- Infection that spreads through the blood vessels and into the brain, resulting in infection, coma, and, in extreme cases, death.
- Infection that affects the entire mouth and face, ultimately obstructing the airways
- Complications from preexisting conditions, such as diabetes.
Some Causes Of Periodontal Abscesses
Abscesses of the gums are opportunistic infections. Even healthy mouths harbor millions of microorganisms. This bacteria is capable of causing infection, but it requires a habitat. Small crevices in the teeth are the most common entry point for bacteria into the mouth.
Main Causes
There are numerous potential causes for these cracks, including:
- Bruxism: Clenching and grinding of the teeth erodes enamel and can lead to fissures.
- An injury to the teeth can create fissures or crevices in which bacteria can thrive.
- Previous dental work: The susceptibility to periodontal abscess of teeth that have had previous cavities filled or dental restorations such as crowns is heightened for teeth that have had prior cavity fillings or restorations.
Other Causes
Poor oral hygiene continues to be a significant risk factor for periodontal abscess. When teeth are not frequently brushed and flossed, bacteria can accumulate. More germs increase the likelihood of infection.
Another risk factor is a diet strong in sugar, acid, and fat. The dental decay-causing bacteria thrive on sugar, acid, and fat. Feeding it excessive amounts of soda, sweet candies, and processed foods will only make it more difficult to eradicate bacteria by brushing and flossing.
How To Treat Periodontal Abscess?
Treatment of a periodontal abscess is necessary to prevent further complications and health problems. If you have a dentist visit but they feel it is safe to wait two days, rinsing your mouth with an Epsom salt solution can assist to clean it.
A cold tea bag and non-steroidal anti-inflammatory medicines (NSAIDs) purchased over the counter can provide temporary pain relief while you wait to visit a dentist.
Periodontal abscess treatment generally follows the same steps as other types of dental abscesses once you arrive at your dental appointment.
Step 1. Drain The Abscess
The abscess will be drained by your dentist in order to eliminate any infectious material and pus. They will next clean the affected region thoroughly with a saline solution.
Step 2: Carry Out a Root Canal
In the majority of instances, root canal therapy can remove diseased and damaged tissue.
Your dentist will use a drill to remove all damaged or dead tissue as well as any irreparable bone. The dentist will then seal and fill the tooth.
Step 3: Extract The Tooth
If the tooth has been subjected to multiple dental abscesses and is so degraded that it will be difficult to prevent another abscess, your dentist may recommend extraction.
Step 4: Scaling And Planning
If the tooth has not been extracted, your dentist will perform a subgingival cleaning procedure. This is known as scaling and planning, a procedure that removes infection-causing plaque and bacteria.
Step 5: Prescribing Antibiotics
In certain situations, your dentist may prescribe antibiotics. This is not always necessary, as the infection should have been eliminated by the previous steps.
Follow-up care is essential to your safety and treatment.
Additionally, you should be aware of your test results and maintain a list of the medications you take.
How Can You Care For Yourself At Home?
- Reduce pain and swelling in your face and jaw by applying ice or a cold compress to the outside of your cheek for ten to twenty minutes. Between the ice and your skin, place a small towel.
- Utilize medications safely. Read and adhere to all labels’ instructions.
- If the doctor prescribes you a painkiller, take it exactly as directed.
- If you are not using a prescription painkiller, ask your doctor if you can take an over-the-counter medication instead.
- Take your antibiotics as instructed. Do not stop taking the medication simply because you feel better. Antibiotics must be taken in their whole.
Periodontal Abscess Prevention
- Daily brushing and flossing, as well as regular dental exams, are recommended.
- Consume a nutritious diet and avoid sugary foods and beverages.
- Avoid smoking and chewing tobacco. Tobacco use slows the healing process. It also increases your risk for periodontal disease and oral and throat cancer. Talk to your doctor about stop-smoking programs and medications if you require assistance. These can increase your likelihood of quitting permanently.





